|
Therefore, the broad use of imaging-guided radiotherapy inevitably has problems. Similarly, even the most accurate diagnosis of lymph nodes by PET-CT still has a high false-positive rate. 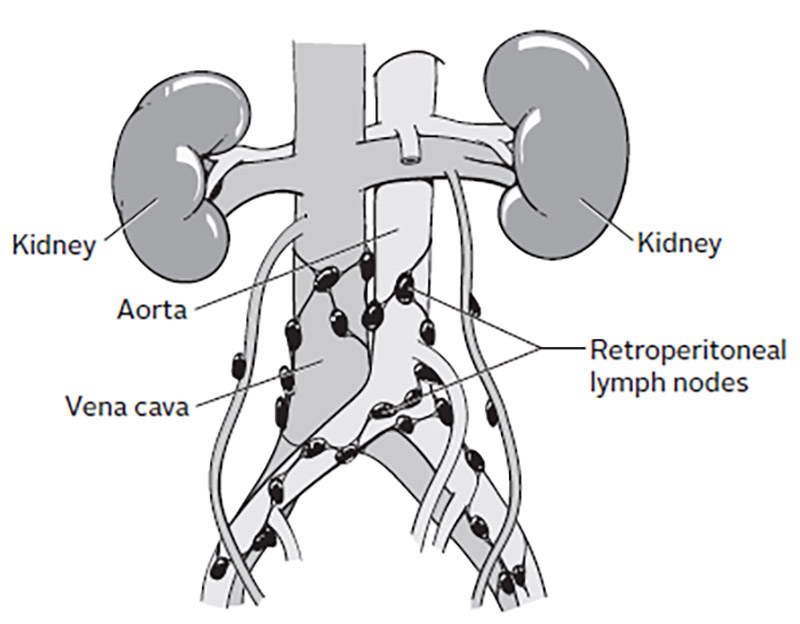
By contrast, the sensitivity and specificity of MRI for judging parametrial infiltration and bladder and rectum invasion are good, but the diagnostic value of metastatic lymph node imaging is limited, with a sensitivity of only 30%. The sensitivity of CT for detecting metastatic lymph nodes is only about 60%. The lymph node status is typically evaluated by computed tomography (CT), magnetic resonance imaging (MRI), and positron emission tomography/computed tomography (PET-CT). The radiotherapy dose and radiation field range determine the therapeutic effect, but inadequate sensitivity and specificity can limit the use of radiotherapy and chemotherapy. 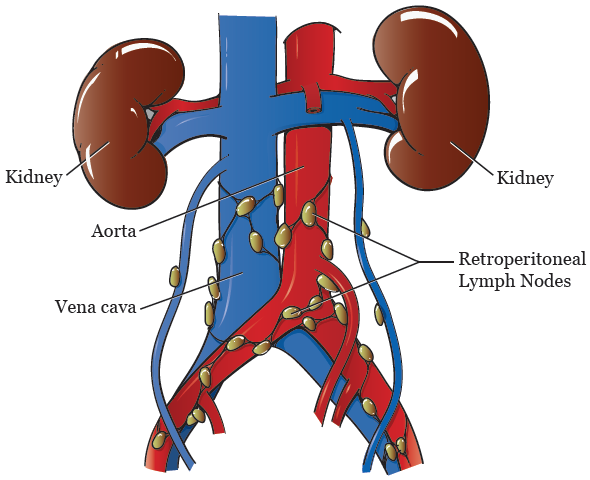
Concurrent chemoradiotherapy is the standard treatment mode for locally advanced cervical cancer. Patients with common iliac lymph node (CILN) and/or PALN metastasis are treated by extended abdominal radiotherapy in the para-aortic lymphatic drainage area. For example, the probabilities of pelvic lymph node (PLN) and para-aortic lymph node (PALN) metastases in patients with stage IB are 11–20% and 2–7%, respectively, and these increase in phase II to 36–45% and 7.2–25%, respectively, while phase III levels reach as high as 40–71% and 21–37%, respectively. Lymph node metastasis is one of the independent prognostic factors for cervical cancer and the lymph node metastasis rate directly parallels the clinical stage. In 2018, the International Federation of Gynecology and Obstetrics (FIGO) officially included the status of lymph node metastasis in the clinical staging of cervical cancer. Patients with MAD < 1.0 cm and SCC-Ag < 5.2 ng/mL may be treated with chemoradiotherapy directly based on imaging, given the low lymph node metastasis rate. Patients with MAD ≥1.0 cm and SCC-Ag ≥ 5.2 ng/mL, as well as high risk factors for CILN and/or PALN metastasis, should undergo resection of enlarged lymph nodes below the common iliac gland and lymphadenectomy of CILN/PALN to reduce tumor burden and to clarify lymph node metastasis status for accurate guidance in follow-up treatment. Correlation analysis showed that non-squamous cell carcinoma, pelvic lymph node (PLN) MAD ≥1.0 cm plus number ≥ 2, and 1 PLN MAD ≥1.0 cm with CILN and/or PALN MAD 0.5–1.0 cm were risk factors for CILN and/or PALN metastasis. The accuracy, specificity, and Youden index of MAD ≥1.0 cm combined with SCC-Ag ≥ 5.2 ng/mL for evaluating lymph node metastasis were 75.71%, 100%, and 0.59, respectively, and were significantly different from the values for the MAD ≥1.0 cm (72.09%, 80.56%, and 0.47, respectively) and SCC-Ag ≥ 5.2 ng/mL (71.43%, 68.97%, and 0.42, respectively) groups. The critical values of MAD and SCC-Ag in determining lymph node metastasis were 1.0 cm and 5.2 ng/mL, respectively. The positive rate of lymph node metastasis was significantly higher in the MAD ≥1.0 cm group (83.33%) than in the 0.5 cm ≤ MAD < 1.0 cm group (26.82%). Overall, 96 patients had 172 visible lymph nodes. The lymph node metastasis rate was 62.50% and the CILN and/or PALN metastasis rate was 31.25%. High-risk factors for common iliac lymph node (CILN) and/or para-aortic lymph node (PALN) metastasis were analyzed. :max_bytes(150000):strip_icc()/retroperitoneal-lymph-nodes-2252167-FINAL-9be89d64f85e476aa092627689f6ce5c.png)
The values of computed tomography lymph node minimum axial diameter (MAD) and squamous cell carcinoma antigen (SCC-Ag), and their combination in predicting retroperitoneal lymph node metastasis were compared. The positive rates of lymph node metastasis were analyzed. Laparoscopic retroperitoneal lymphadenectomy was performed in 96 patients with advanced cervical cancer. This study aimed to explore the choice of these assessment methods. The assessment of retroperitoneal lymph node status in patients with locally advanced cervical cancer is still a problem.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
